Over the last decade, consumer-driven health care elevated customer satisfaction to be the central mission of hospital care. Satisfaction surveys and hotel-style amenities rose hand-in-hand to become central features of U.S. hospitals. This trend has done more harm than good. It focuses everyone’s attention on front-stage aspects of health care over what matters most to patients: excellent medical treatment.
As I discovered in a recent study published in Social Forces with my colleague Xinxiang Chen, satisfaction scores are driven by room and board hospitality, rather than medical quality or patient survival rates. Moreover, when hospitals face greater competition from other facilities, there is higher patient satisfaction, but lower medical quality.
Customer / patient satisfaction scores in medicine are essentially just hospital Yelp reviews. They focus on the things most immediately visible to patients: the front stage of medical care. The sociologist Erving Goffman once wrote that all of social life is a drama split between front stage and back stage worlds. The front stage is a world of observable actions and performance; the other is a place outside the view of an audience.
In hospital care, technical medical treatment is part of the back stage. Most hospital patients are acutely sick or injured, lacking expertise in their diagnosis and treatment, anxious for their health and survival, and heavily medicated. Most patients do not want to think about possible errors in their treatment – though medical mistakes are common enough to be a leading cause of death in the U.S. For patients, the technical details of treatment happen behind a curtain, away from their view.
The front stage of hospitals is the room and board care, and this is exceedingly visible. Patients must be fed (is the food warm, tasteful?), they must sleep (is the room quiet or busy?), they must cope with their immediate pain, anxiety, fears, and frustrations (are the nurses and staff kind and caring, quick to respond to concerns?).
How do patients judge their hospital when these services are so different? Is satisfaction driven mostly by front-stage hospitality – things like quiet rooms and friendly staff – or by the back-stage elements of patient safety and medical excellence?
To study this, my colleague and I analyzed data from more than 3,000 U.S. hospitals. The data come from the Centers for Medicare and Medicaid Services, and include measures of satisfaction, room and board care, medical excellence and patient survival rates.
Patients, it turns out, are extremely responsive to hospitality features. Quiet, tidy rooms matter much more for satisfaction than either technical medical quality or patient survival. Personal interaction with nurses is the single biggest driver. Hospitals showing great rapport with nurses score 27 points higher on satisfaction.
Of course, nurses play a central role in medical quality. But patients and satisfaction surveys seem to judge them by the standard of a friendly personal assistant. This is why nurses today have scripts telling them exactly what friendly words to use with patients so as to maximize the hospital’s scores.
Hospitals with the best records of medical quality and safety standards, however, have scarcely higher customer satisfaction scores. Consider a hospital’s safety record: the death rate, adjusted for patient mix. Hospitals with the worst death rates do have – as one would hope – lower satisfaction scores, but only 2 points below hospitals with the very best record of patient survival (62 percent satisfaction, versus 64 percent). Nurse communication has ten times more effect than overall patient survival.
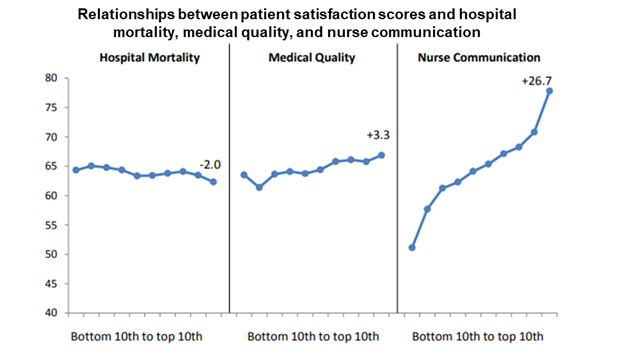
When patients enter an acute care hospital, often their deepest fear is that they might die there. Yet hospital death rates matter little for satisfaction scores. Consumer focus is tuned to things that customers can instantly perceive. The things that save their lives are much harder to perceive and evaluate.
To investigate this further, we conducted a second analysis of hospitals where we could see their competitive environment. In many places in the country, there is a high concentration of hospitals striving to serve the same pool of patients. Such hospitals “have found themselves in a fierce fight… pitted against other hospitals, pulling out all stops to maintain market share” as Griffin documents. Across multiple measures of hospital competition, we find that high competition for patients leads to higher satisfaction scores, but lower medical quality.
This suggests that when competition for patients is more intense, hospitals focus on front-stage hospitality rather than back-stage medical excellence or patient safety.
Market advocates have long argued that “health care will not improve until consumers are driving it” as Herzlinger wrote. In contrast, it seems likely that the consumerist orientation is decoupling care from the best interests of patients. Today, we are rating, ranking, and managing hospitals based on the factors that are least important for patients’ health and longevity. As a health care business strategy, investing in front stage amenities promises much higher satisfaction payoffs than medical quality.
Indeed, hospitals have for years focused on developments like 24-hour room service, gourmet meals, designer hospital gowns, and immense capital investments in private rooms and luxury amenities – waterfalls and Wi-Fi, grand pianos in the lobby, artwork, ‘healing’ gardens, and atriums with views of the bay. One hospital executive in Los Angeles summarized it well: “[the hospital] looks like you’re in a country club… I think it gives people hope.”
There is a new kind of “buyer beware” philosophy in medicine. If hospitals are doing what raises satisfaction scores, customers must be getting what they wanted. But, this is deeply troubling when satisfaction scores show not what patients value the most, but simply what they can see in their hospital.
This does not serve the best interests of patients nor reflect their deepest hopes for their treatment.
Build back better
Even before the pandemic, life expectancy in America declined for three out of the previous four years. There is now a striking gap in health outcomes between Americans and citizens of other western countries. Even high-income Americans with insurance have shorter lives and poorer health than their peers abroad.
Rather than facing head on our problems of health and longevity, the U.S. has focused on making hospitals a better consumer product. The vision of consumer-driven health care turns hospitals into hotels.
The pandemic reminds us that hospitals are an essential service to the community, and that no one is safe from devastating illness. The metrics of hospital success should not be customer satisfaction and whatever is most visible to patients. As we begin to build back better, we need renewed focus on the back-stage achievements of medical excellence, patient safety and survival: the things we ultimately want from our medical providers.
Read more
Cristobal Young and Xinxiang Chen. “Patients as Consumers in the Market for Medicine: The Halo Effect of Hospitality.” in Social Forces 2020.
Image: sasint via pixabay

No Comments